📌 Key Takeaways
Sleep hygiene alone often plateaus when insomnia becomes chronic, leaving you guessing whether tonight will be restful or another frustrating wake-up cycle.
- Pairing Creates Predictability: Combining solid sleep routines with a physician-supervised, non-controlled medication taken at a consistent time each night narrows the variability between good and bad nights.
- Timing Matters as Much as Dose: Taking your medication within the same 30 to 60 minute window before bed helps it clear your system by morning, reducing grogginess that many people mistakenly blame on the medication itself.
- Non-Controlled Means Lower Risk: Medications like trazodone, hydroxyzine, and clonidine have significantly lower abuse potential than controlled substances, making them safer options for long-term insomnia management under medical supervision.
- Pattern-Fit Selection Improves Results: Matching your medication to whether you struggle with falling asleep versus staying asleep—rather than using a one-size-fits-all approach—addresses your specific sleep disruption more effectively.
- Simple Self-Tracking Drives Adjustments: Rating your morning clarity on a 1 to 10 scale gives you and your clinician real-world feedback to fine-tune timing before jumping to dose changes.
Predictable nights come from predictable steps: the right medication, the right timing, and the right habits working together.
Tech-savvy working adults between 25 and 44 who maintain good sleep habits but still struggle with persistent insomnia will find this practical framework here, preparing them for the detailed comparison and implementation guidance that follows.
~~~~~~~~~~~~~~~~~~~~~
You’ve done everything right. The bedroom is cool and dark. Your phone stays in the other room after 9 PM. You stopped drinking coffee after lunch. Yet here you are at 2:37 AM, staring at the ceiling, running through tomorrow’s presentation for the third time tonight.
Sound familiar? You’re not alone in this frustration. Many people maintain excellent sleep habits—what doctors call “sleep hygiene”—and still struggle with persistent insomnia. The routines help, but they don’t always solve the problem on their own.
This is where a different approach makes sense: pairing those solid habits with a supervised, non-controlled sleep medication. When you combine basic routines with the right medication taken at the right time, plus a simple list of things to avoid, you create a more predictable pattern. The variability that keeps you guessing each night starts to decrease, and your mornings become clearer.
Understanding the Basics: Definitions That Matter
Sleep hygiene refers to the behavioral and environmental practices that promote consistent, quality sleep. This includes maintaining a regular sleep schedule, creating a comfortable bedroom environment, limiting caffeine and alcohol, and establishing a calming pre-bed routine. Research shows these foundational practices support your body’s natural sleep-wake cycle.
Non-controlled sleep medications are physician-prescribed options that have significantly lower abuse potential than controlled substances. These include medications like trazodone, hydroxyzine, and clonidine—effective drugs that help regulate sleep without the high dependency risk associated with benzodiazepines or Z-drugs (Ambien, Lunesta). While these medications should always be used under medical supervision, they’re widely considered safer alternatives for long-term insomnia management.
Think of it this way: imagine you’re trying to unlock a tricky door. Sleep hygiene is like making sure the door is properly aligned in its frame—essential groundwork. The medication is the key that turns the lock. But you still need steady hands (that’s your timing window) to make everything work smoothly together.
Here’s what this looks like in practice: You notice you’ve been lying awake for 45 minutes or more on most nights, despite your consistent wind-down routine. A supervised approach adds a timed medication—taken in a specific 30 to 60 minute window before bed—combined with an “on-med checklist” that protects your results. You track how you feel each morning using a simple self-assessment, then make small adjustments with clinician guidance if needed.
This pairing model addresses the core issue: when insomnia becomes entrenched, good habits alone often can’t break the cycle. Predictable nights come from predictable steps.
Why Sleep Hygiene Alone Often Stalls
Good Habits Don’t Equal Fixed Results When Insomnia Is Entrenched
Sleep hygiene works beautifully for many people. If you’re occasionally restless or adjusting to a new schedule, cleaning up your bedtime routine might be all you need. The research is clear: maintaining consistent sleep and wake times, avoiding stimulants late in the day, and creating a dark, quiet sleep environment all support better rest.
But here’s what happens when insomnia becomes chronic. Your nervous system gets stuck in a heightened state. Even when every external condition is perfect—room temperature just right, no noise, zero distractions—your brain won’t downshift into sleep mode. You’ve conditioned yourself to associate the bed with wakefulness and frustration rather than rest.
According to the National Institute of Mental Health, sleep problems and mental health are closely linked, and chronic sleep issues can create a self-reinforcing pattern that behavioral changes alone struggle to interrupt.
Where Hygiene Shines—and Where It Plateaus
Sleep hygiene excels at creating the right conditions for sleep. It removes obstacles. It sets up your environment and schedule to support your body’s natural rhythms. For people with mild, situational sleep problems, these changes often provide complete relief within a few weeks.
The plateau happens when the problem goes deeper. If you’ve had trouble falling or staying asleep for months or years, the issue isn’t just about your environment anymore. Your sleep drive might be dysregulated. Your stress response might be overactive at night. You might have developed anxiety specifically around bedtime, creating a mental barrier that good habits can’t fully address.
This is where hygiene becomes necessary but not sufficient. You need something that works on a different level—something that helps reset the underlying patterns while you maintain those helpful routines.
What Changes When You Add a Non-Controlled Med (Supervised)
Pattern-Fit Choices: Matching Medication to Your Specific Sleep Problem
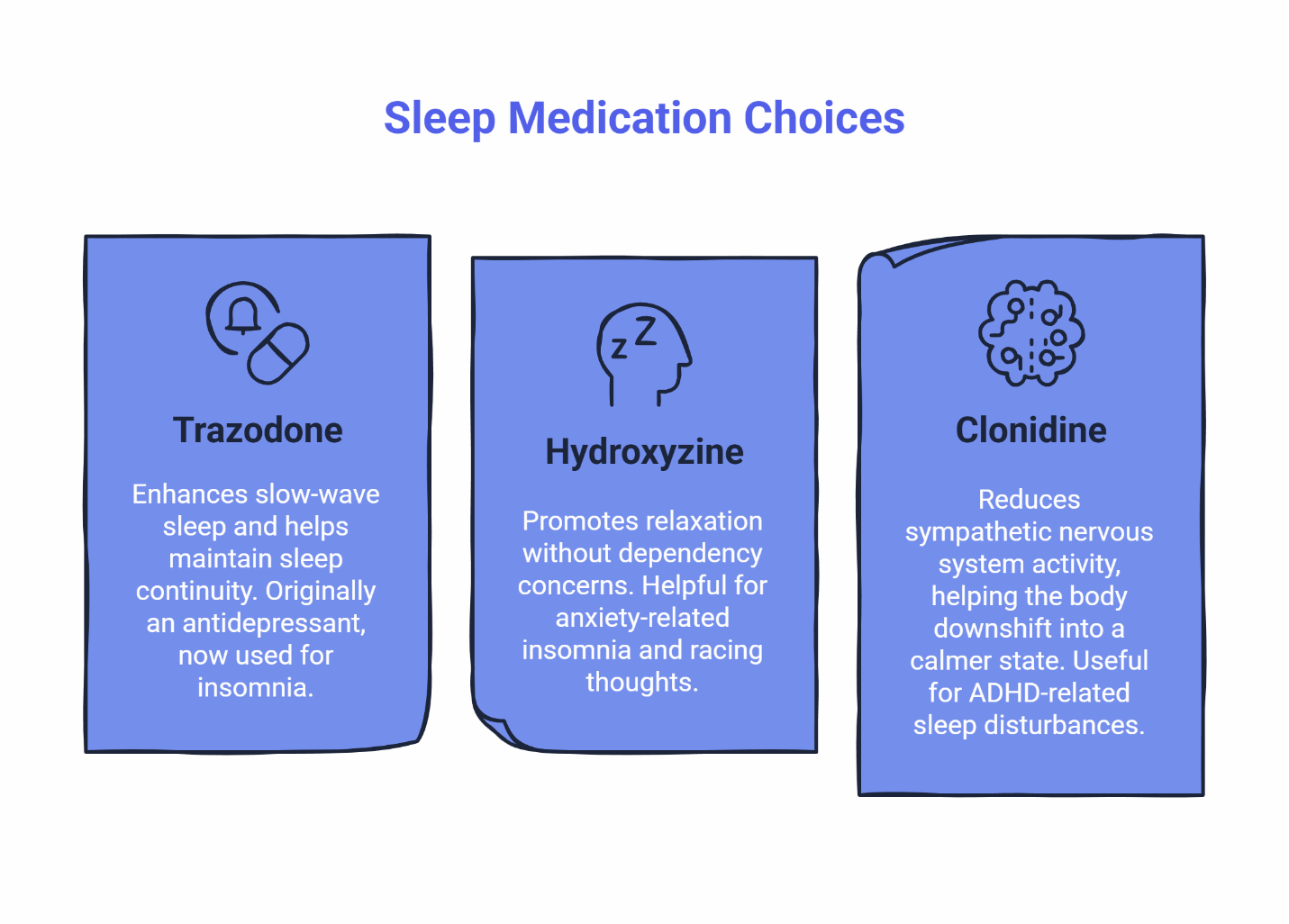
Not all sleep problems look the same, which is why physicians consider your specific pattern before recommending a medication. Do you struggle mainly with falling asleep, or do you wake up repeatedly during the night?
Trazodone is often chosen for people who have trouble staying asleep. It enhances slow-wave sleep—the deepest, most restorative phase—and helps maintain sleep continuity throughout the night. Originally developed as an antidepressant, it’s now widely used off-label for insomnia because it’s effective and has a lower abuse potential than controlled sleep medications. Learn more about trazodone.
Hydroxyzine works well for anxiety-related insomnia. It’s an antihistamine that promotes relaxation without the dependency concerns of controlled substances. Many people find it particularly helpful when racing thoughts or general restlessness prevent sleep onset. Its calming effects help both with falling asleep and staying asleep.
Clonidine addresses the overactive nervous system that keeps some people wired at night. Originally a blood pressure medication, it reduces sympathetic nervous system activity—essentially helping your body downshift into a calmer state that’s more conducive to sleep. It’s especially useful for people with ADHD-related sleep disturbances or those who feel their mind and body can’t settle down.
Each medication has a distinct mechanism, and your physician will consider your complete picture—including any other health conditions, medications you’re taking, and your specific sleep pattern—when making a recommendation. You can explore detailed information about each option on our Medication Selection page.
Timing Windows Reduce Next-Day Fog
This might be the most underappreciated aspect of using sleep medication effectively. Both the dose and timing matter for how you feel the next morning, but timing is often the easier variable to adjust first.
A timing window means taking your medication consistently within the same 30 to 60 minute period before your target bedtime. This isn’t arbitrary. Your body processes medication at a predictable rate. When you take it at roughly the same time each night, you create a reliable pattern. The medication peaks when you need it most—during those first few hours of sleep—and clears your system by morning.
Many people experiencing grogginess focus immediately on changing their dose, but timing plays a surprisingly large role. Taking your medication too late means it’s still active when your alarm goes off. Taking it inconsistently—10 PM one night, midnight the next—prevents your body from establishing a rhythm. Before adjusting your dose, it’s worth exploring whether a timing shift resolves the issue.
Research emphasizes that consistency in sleep timing is fundamental to healthy sleep architecture. This same principle applies to medication timing: consistency reduces variability and side effects.
For a deeper look at how timing affects morning clarity, read our article on timing matters.
The Pairing Model: Med + Routine = Predictable Nights
The “First 7 Nights” Loop: Building Your Sleep Auto-Pilot
The first week is when you establish your baseline. This isn’t about perfection—it’s about creating a simple, repeatable system that you can adjust based on real feedback.
Here’s the framework:
Start with your fixed wind-down routine about an hour before bed. This signals to your body that sleep is approaching. Then, within your designated timing window (let’s say 10:00 to 10:30 PM if your target bedtime is 11 PM), you take your medication.
Each morning, you assess how you feel using a simple self-rating from 1 to 10. We call this your morning clarity check. This isn’t a scientifically validated instrument—it’s a straightforward communication tool we’ve developed to help you and your clinician track your subjective sense of how alert and refreshed you feel when you wake up.
- 7 or above: Good result. Maintain your current timing.
- Below 7 for two consecutive days: Time to adjust. This usually means shifting your dose time 15 to 30 minutes earlier.
- Red-flag symptoms (severe grogginess, dizziness, or any concerning reaction): Contact your clinician immediately.
This feedback loop helps prevent the common mistake of changing your dose when you actually need to change your timing. While both dose and timing affect how you feel, timing adjustments are often the first step in fine-tuning your results. For practical guidance on managing these first-week adjustments, see our guide on managing morning grogginess.
The On-Med Checklist: What to Avoid to Protect Your Results
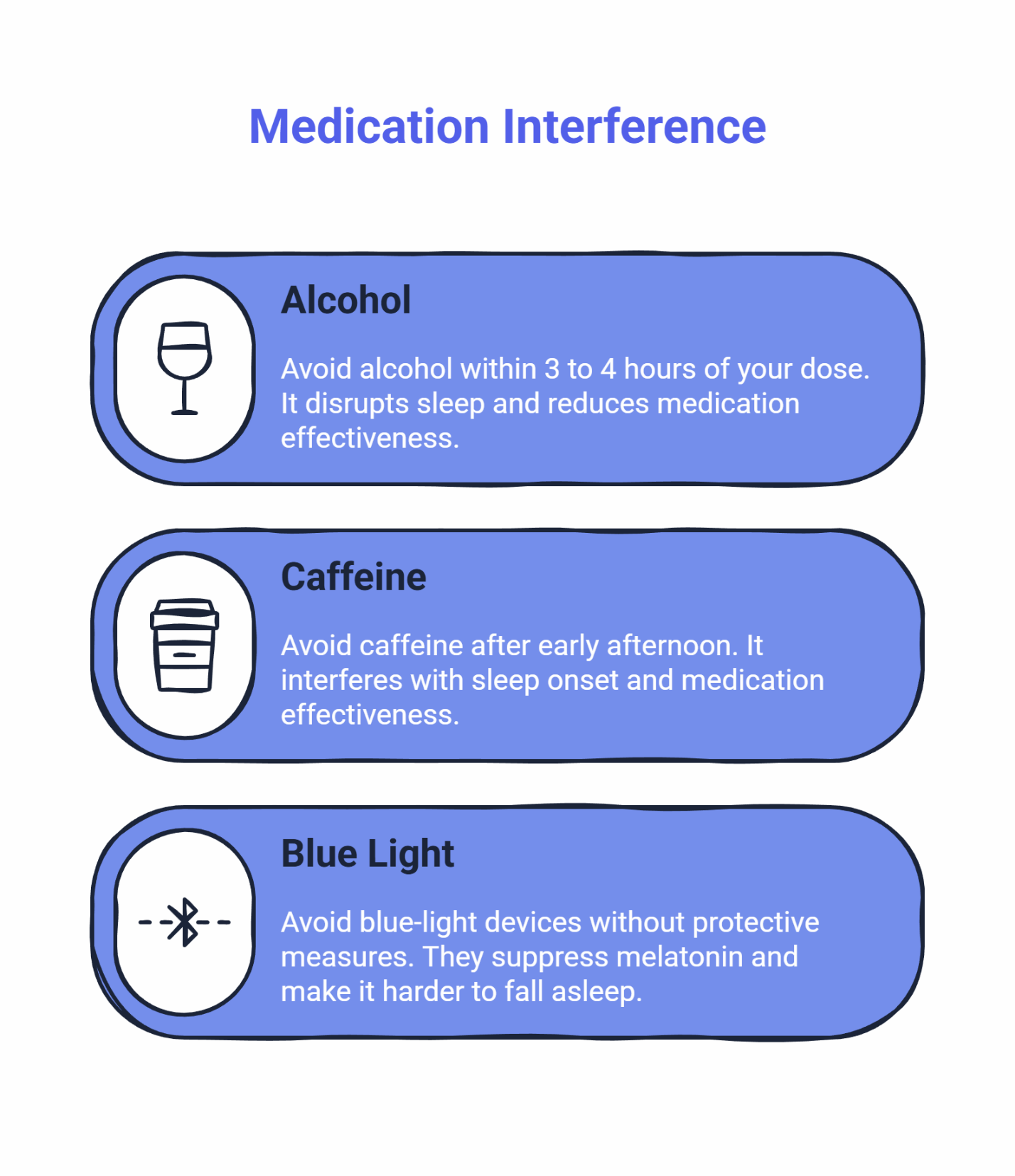
Medication doesn’t work in isolation. Certain substances and behaviors can interfere with its effectiveness or increase side effects. Protecting your results means avoiding three main culprits:
Alcohol within 3 to 4 hours of your dose. Alcohol might make you drowsy initially, but it fragments your sleep later in the night. Research shows that alcohol disrupts sleep architecture, particularly REM sleep, even in moderate amounts. When combined with sleep medication, it can intensify morning grogginess and reduce the medication’s effectiveness.
Caffeine after early afternoon. Caffeine has a half-life of about 5 to 6 hours, meaning it takes that long for your body to eliminate half of what you consumed. A cup of coffee at 3 PM still has a quarter of its caffeine in your system at 9 PM, potentially interfering with both sleep onset and the medication’s effectiveness.
Blue-light devices without protective measures. Bright screens suppress melatonin production, making it harder to fall asleep even with medication on board. If you must use devices in the evening, enable night mode or warm color settings, and stop at least 30 minutes before taking your medication.
These aren’t extreme restrictions. They’re practical boundaries that allow the medication and your natural sleep drive to work together rather than fight each other.
Using Your Morning Self-Assessment to Fine-Tune Results
Your morning self-rating is a simple but useful tool. Here’s how to use it effectively with your clinician’s guidance:
If your score is 7 or above most mornings:
- You’re achieving good results. Continue your current timing window and routine.
If your score stays between 4 and 6 for two or more consecutive days:
- You’re getting sleep, but waking up too sluggish. This usually signals a timing issue. Ask your clinician about shifting your medication window 15 to 30 minutes earlier. This allows the medication more time to clear your system before you need to be alert. Depending on your situation, your clinician may also consider whether a dose adjustment is appropriate.
If your score drops to 3 or below, or you feel unsafe to drive or work:
- Contact your clinician to discuss adjustments. This level of impairment suggests your current plan needs modification—possibly a different timing strategy, dose adjustment, or medication change.
If you notice unusual symptoms:
- Severe dizziness, breathing changes, chest pain, or neurological symptoms require immediate attention. Contact your clinician or seek urgent care rather than trying to adjust on your own.
This systematic approach helps you and your clinician work together to optimize your treatment plan based on your real-world experience.
Safety-First, Low-Friction Care: How to Start
Asynchronous Intake Where Permitted: Fast, Physician-Approved Process
We’ve designed our intake process to remove unnecessary barriers while maintaining safety standards. Where permitted by state law, you can complete your entire evaluation online without scheduling a live appointment.
Here’s how it works: You answer a structured questionnaire about your sleep history, current medications, and overall health. This information goes directly to a licensed physician who reviews it—typically within hours. If you’re eligible and your case is straightforward, the physician approves your treatment plan and sends a prescription electronically to your chosen pharmacy. Many eligible patients receive their prescription the same day they complete the intake.
This approach works because we’ve built safety screening directly into the process. The questionnaire flags any medical or psychiatric conditions that would require more detailed evaluation or make online treatment inappropriate. Real doctors review every case. Nothing is automated when it comes to prescription decisions.
You can get started with your evaluation here.
When We Require a Brief Virtual Visit
Some situations need a live conversation. This isn’t about making the process more complicated—it’s about providing safe, appropriate care.
State regulations vary significantly. Some states require a synchronous (real-time) provider interaction before any prescription can be issued for telemedicine patients. If your state has this requirement, we’ll schedule a brief video or phone visit within three business days. These regulations change periodically, so the process you experience will reflect current legal requirements in your location.
Complex medical histories also trigger the need for a virtual visit. If you’re taking multiple medications, have significant health conditions, or if your sleep problem presents with unusual features, a physician will want to discuss your situation directly. This ensures we’re not missing something important and that the treatment plan truly fits your needs.
These visits are typically 10 to 20 minutes—long enough to get clarity, short enough to respect your time. To understand the difference between our asynchronous and virtual care options, visit our comparison page.
Eligibility Window: Who We Can Treat Safely Online
Telemedicine has boundaries, and we’re transparent about them. We can safely treat adults aged 18 to 65 who don’t have major medical, mental health, or substance use conditions that would make sleep medications risky.
We cannot treat you online if:
- You’re pregnant or planning to become pregnant
- You have significant psychiatric conditions requiring specialized management
- You’re currently taking daily benzodiazepines or other controlled sleep medications
- You have severe, uncontrolled medical conditions
These restrictions aren’t arbitrary. They reflect both medical safety considerations and the limitations of virtual care. Some conditions require hands-on evaluation or closer monitoring than online treatment can provide.
If you’re unsure whether you qualify, the quickest way to find out is to start the intake. The process will screen for eligibility issues and let you know if you’re a good fit for our service. If you have unique circumstances that might affect eligibility, you can reach out to us at Admin@SleepScriptMD.com.
For complete eligibility details, see our Getting Started page.
When Hygiene-Only Is Enough (and When It Isn’t)
If you’ve been sleeping well lately—falling asleep within 20 minutes most nights, staying asleep through the night, waking up feeling reasonably refreshed—then stick with what’s working. Maintain your good habits. You don’t need medication if your current approach is producing the results you want.
But if you’ve been working on your sleep hygiene for weeks or months and still find yourself lying awake regularly, or if you’re waking up multiple times each night despite following all the “rules,” it’s worth considering a different approach.
The key question isn’t “Have I tried hard enough with hygiene?” It’s “Am I getting the predictable, restorative sleep I need to function well during the day?”
Persistent insomnia—defined as difficulty falling or staying asleep at least three nights per week for three months or more—often requires intervention beyond behavioral changes. This doesn’t mean you’ve failed at sleep hygiene. It means your nervous system needs additional support to break out of an entrenched pattern.
A supervised, non-controlled medication paired with your existing routine can provide that support. It’s not about replacing good habits; it’s about building on them to achieve more consistent results.
Red-Flags and Conditions We Don’t Treat Online
Some sleep disorders require in-person evaluation and testing that goes beyond what telemedicine can provide. We want you to get the right care, even if that means we’re not the right provider for your situation.
Narcolepsy: Sudden Sleep Attacks and Cataplexy
Narcolepsy is a neurological condition, not just severe insomnia. Warning signs include:
- Falling asleep unexpectedly during the day, sometimes during conversations or while driving
- Sudden muscle weakness triggered by strong emotions (laughing, anger, surprise)
- Feeling paralyzed when falling asleep or waking up
- Extremely vivid dreams or hallucinations at sleep transitions
These symptoms indicate a serious disorder that requires specialized testing—typically an overnight sleep study followed by a multiple sleep latency test. This isn’t something we can diagnose or treat through our platform. If these symptoms sound familiar, please seek evaluation from a local sleep specialist or neurologist. The Narcolepsy Network offers resources and support for finding appropriate care.
REM Sleep Behavior Disorder: Acting Out Dreams
During normal REM sleep, your muscles are temporarily paralyzed to prevent you from moving while you dream. In REM Sleep Behavior Disorder (RBD), this protective mechanism breaks down. People with RBD may yell, kick, punch, or thrash during sleep, sometimes injuring themselves or their bed partner.
This condition requires proper diagnosis before beginning any sleep treatment. RBD can be an early indicator of certain neurological conditions, particularly in older adults, which is why we refer patients with these symptoms for in-person evaluation. Diagnosis requires video polysomnography (an overnight sleep study) at a sleep center. If you or your partner has noticed you acting out dreams, please consult a neurologist or local sleep specialist.
Restless Legs Syndrome: Uncomfortable Urges to Move
Restless Legs Syndrome (RLS) causes uncomfortable sensations in the legs, usually worse at night or while resting, creating an irresistible urge to move. While sometimes benign, RLS can signal underlying conditions that need evaluation:
- Iron deficiency (with or without anemia)
- Kidney disease
- Peripheral nerve damage (from diabetes, B12 deficiency, or alcohol use)
- Neurological conditions like Parkinson’s disease or multiple sclerosis
- Medication side effects from antihistamines or certain antidepressants
Because RLS often has a correctable underlying cause, it requires blood work and in-person evaluation before treatment. Please follow up with your primary care provider or a local specialist for testing that may include ferritin, iron levels, kidney function, B12, and blood sugar.
Sleep Apnea: Snoring, Gasping, or Breathing Pauses
If you’ve been told you snore loudly, gasp for air, or stop breathing during sleep, proper evaluation for obstructive sleep apnea (OSA) is essential before starting any sleep medication. OSA is a condition where your airway repeatedly collapses during sleep, causing breathing interruptions.
We follow evidence-based clinical protocols: when sleep apnea is suspected, we arrange an at-home sleep test first. This ensures your breathing is properly assessed before beginning insomnia treatment. Once your test results are reviewed, or if you’re already successfully treating diagnosed sleep apnea with CPAP therapy, we can proceed with your insomnia care plan.
Share This Plan in 30 Seconds
Want to explain this approach to your partner quickly? Here are the key points:
- The pairing model: Good sleep habits plus a non-addictive, physician-prescribed medication taken at a consistent time each night creates more predictable results than either approach alone.
- Safety-first: We only prescribe non-controlled medications with lower abuse potential than controlled substances. A physician reviews every case. Some conditions require in-person evaluation instead.
- The timing window: Taking medication consistently within the same 30 to 60 minute period before bed, plus following a simple “avoid list,” helps reduce morning grogginess and improves results.
- When to reach out: If you notice red-flag symptoms or have concerns during the first week, contact your clinician immediately—earlier is better.
Try This Today: Fast On-Ramps
Start with a Quick Assessment
Not sure if you need additional support beyond sleep hygiene? Take one of our free screening quizzes to get clarity:
The 6-Second Sleep Check — Just 5 questions. Flags insomnia, fatigue, and snoring risk. Perfect if you’re in a hurry and want a quick gut check.
The 2-Minute Sleep Clarity Quiz — About 9 questions based on clinical sleep assessment tools. This is the best balance of insight and speed for most people. It helps you understand what’s specifically affecting your rest.
The Deep Sleep Profiler — A comprehensive screening that takes 3 to 5 minutes. This covers insomnia, apnea risk, narcolepsy indicators, and more. Choose this if you’ve tried multiple approaches and need a complete breakdown with clear next steps.
Understand Your Options and Start When You’re Ready
Once you have a clearer picture of your sleep pattern, you can explore your treatment options:
Check our Pricing page to see exactly what the service costs. We don’t bill insurance, which keeps the process simple and transparent. Most of the medications we prescribe are generic and affordable at your local pharmacy.
Compare AI-Assisted vs. Virtual Care to understand which path makes sense for you. Most patients start with our asynchronous option for speed and convenience where their state permits it. Those with more complex medical histories or who prefer direct provider interaction can choose a virtual appointment.
Ready to begin? Start your evaluation here. The process walks you through eligibility screening and intake. If you’re eligible, you’ll typically have a prescription within hours in states that allow asynchronous prescribing.
Already a patient? Visit our Returning Patients page for refills, medication adjustments, or support questions.
Frequently Asked Questions
Do non-controlled sleep medications cause addiction?
The medications we prescribe—trazodone, hydroxyzine, and clonidine—are classified as non-controlled because they have significantly lower abuse potential compared to controlled substances like benzodiazepines or Z-drugs. While these medications should always be used under medical supervision and some people may experience mild withdrawal symptoms if stopped abruptly, they don’t carry the same dependency risks as controlled sleep medications. Learn more about how non-controlled sleep medications work.
Will I feel groggy in the morning?
Morning grogginess can be influenced by both timing and dose. Many people find that taking their medication consistently within the same 30 to 60 minute window before bed helps minimize next-day effects. If you do experience grogginess, small adjustments—typically shifting your dose time 15 to 30 minutes earlier—often resolve it. Your clinician can guide these adjustments and may also consider whether a dose modification is appropriate. Read more about managing morning grogginess.
How fast can I start treatment online?
Where state law permits asynchronous prescribing, eligible patients can often receive their prescription the same day they complete their intake. Some states require a brief video visit before prescribing, which we can typically schedule within three business days. The speed depends primarily on your state’s current telemedicine regulations and your individual medical situation.
Am I eligible for online treatment?
We can safely treat adults aged 18 to 65 who don’t have major medical conditions, active psychiatric disorders, or substance use issues that would make sleep medications risky. We cannot treat pregnant women or those planning pregnancy. If you’re unsure, start the intake process—it includes eligibility screening and will let you know if you’re a good candidate. For specific questions about unique circumstances, email Admin@SleepScriptMD.com.
What if I snore or stop breathing during sleep?
We follow clinical best practices: when sleep apnea is suspected, we arrange an at-home sleep test before starting insomnia medication. Once we have your test results and understand your breathing during sleep, we can proceed with appropriate treatment if needed.
Is hygiene enough for chronic insomnia?
Hygiene provides essential support for sleep, but if you’ve been struggling with persistent difficulty falling or staying asleep for months despite maintaining good habits, a supervised non-controlled medication plus timing optimization often produces more consistent results. The combination addresses both the behavioral and physiological aspects of chronic insomnia.
How much does this service cost?
Pricing is transparent and straightforward. We don’t bill insurance, which eliminates confusion about coverage and claims. For current rates and details about our asynchronous care and virtual visit options, visit our Pricing page. The medication costs are separate and paid at your pharmacy, where many insurance plans may provide coverage.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. A physician must evaluate your individual situation before prescribing any medication. Not all patients are eligible for our service due to medical, psychiatric, or regulatory considerations. Some states require a synchronous video visit before prescribing sleep medications via telemedicine.
Our Editorial Process
Content created by SleepScriptMD is developed by our clinical team and reviewed for accuracy by licensed physicians. We base our guidance on current medical literature, clinical experience, and evidence-based treatment approaches. Our goal is to provide clear, helpful information that supports informed decision-making about sleep health.
SleepScriptMD Insights Team
We believe in making effective, non-addictive sleep treatment accessible and straightforward. Our platform connects patients with licensed physicians who provide evidence-based care designed for modern life.
