📌 Key Takeaways
Night-shift workers can soften daylight saving time disruptions by starting small timing adjustments two to three days before the clock changes.
- Start Adjusting Early: Shift your sleep, meals, and caffeine cutoff by 15–30 minutes daily starting three days before DST hits.
- Protect Your First Sleep Block: The recovery sleep right after the time change matters most—darkness, consistency, and enough time in bed are your priorities.
- Use Light Strategically: Bright light early in your shift helps alertness; sunglasses on the drive home protect your wind-down.
- Track Your Recovery: Note how easily you fall asleep, how clear you feel waking up, and whether grogginess lingers past a few days.
- Know When It’s More Than DST: Snoring, gasping, acting out dreams, or restless legs signal conditions that need proper evaluation, not just schedule tweaks.
Gradual prep beats last-minute scrambling every time.
Night-shift nurses, factory workers, first responders, and rotating-schedule employees will find practical timing strategies here, preparing them for the detailed prep timeline that follows.
~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~ ~
The clock jumps forward. You’re still on shift.
Your body was already confused about when to sleep. Now the rest of the world just moved an hour in a direction your schedule doesn’t follow. For night-shift workers, daylight saving time isn’t a minor inconvenience that a strong cup of coffee can fix. It’s a predictable hit to a system that’s already working overtime to keep you functional.
The good news: this is manageable. A short prep plan started a few days before the change can soften the impact significantly. This guide walks through exactly what to do before, during, and after the DST switch so you’re not white-knuckling through another rough week.
In the United States, daylight saving time begins on the second Sunday in March and ends on the first Sunday in November. The direction of the change affects your approach. In spring, you lose an hour. In fall, you gain one. Either way, the smartest move is to start adjusting two to three days before the clock changes, not after you feel wrecked by it. NIST maintains the official reference for these dates.
Why Daylight Saving Time Hits Night Shifts Harder
What “Double Misalignment” Means
Night-shift workers deal with double misalignment. Shift work already puts sleep and work hours in tension with the normal light-dark cycle that helps guide circadian rhythms. Then DST adds another abrupt timing change on top of that.
Most DST advice assumes you sleep when it’s dark and wake when it’s light. That advice doesn’t land the same way when your schedule already runs opposite to the sun.
Working overnight means your internal clock is constantly fighting external cues. Your body wants to sleep when it’s dark, but you’re awake. It wants alertness during daylight, but that’s when you’re trying to rest. According to NIOSH training materials, shift workers experience ongoing tension between their work schedule and the light-dark cycle that naturally regulates sleep.
DST adds another layer. When the clocks change, you’re not just dealing with the normal shift-work misalignment. You’re stacking an external time shift on top of an already disrupted circadian rhythm. That’s double misalignment, and it explains why the same one-hour change that slightly annoys your day-shift friends can throw off your sleep for a week.
Why the Same One-Hour Change Feels Bigger When Your Bedtime Already Moves
A daytime worker loses an hour of sleep one night, feels groggy the next morning, and mostly adjusts within a day or two. Their sleep window and the external clock still move in the same direction.
For night nurses, factory workers, first responders, and rotating-shift employees, the math is messier. Your sleep window might already shift depending on your rotation. Your exposure to morning light, which normally helps reset the clock, happens when you’re trying to wind down. And the DST change doesn’t care that you just worked 12 hours.
Circadian disruption causes drowsiness, poor coordination, and trouble focusing in the short term. The National Institute of General Medical Sciences explains how biological clocks regulate these functions and how disruption affects performance. That’s a big deal when your job already asks you to stay sharp at biologically awkward hours.
The result: the adjustment period often stretches longer, the grogginess feels heavier, and the risk of alertness problems at work—or drowsy driving on the way home—goes up.
The objective is mitigation, not total elimination of the disruption.
Your DST Prep Timeline
Small, deliberate timing changes over several days work better than one abrupt adjustment. NIOSH specifically notes that one way to help the body adjust is to gradually change the times for sleep, eating, and activity. Here’s how to break it down.
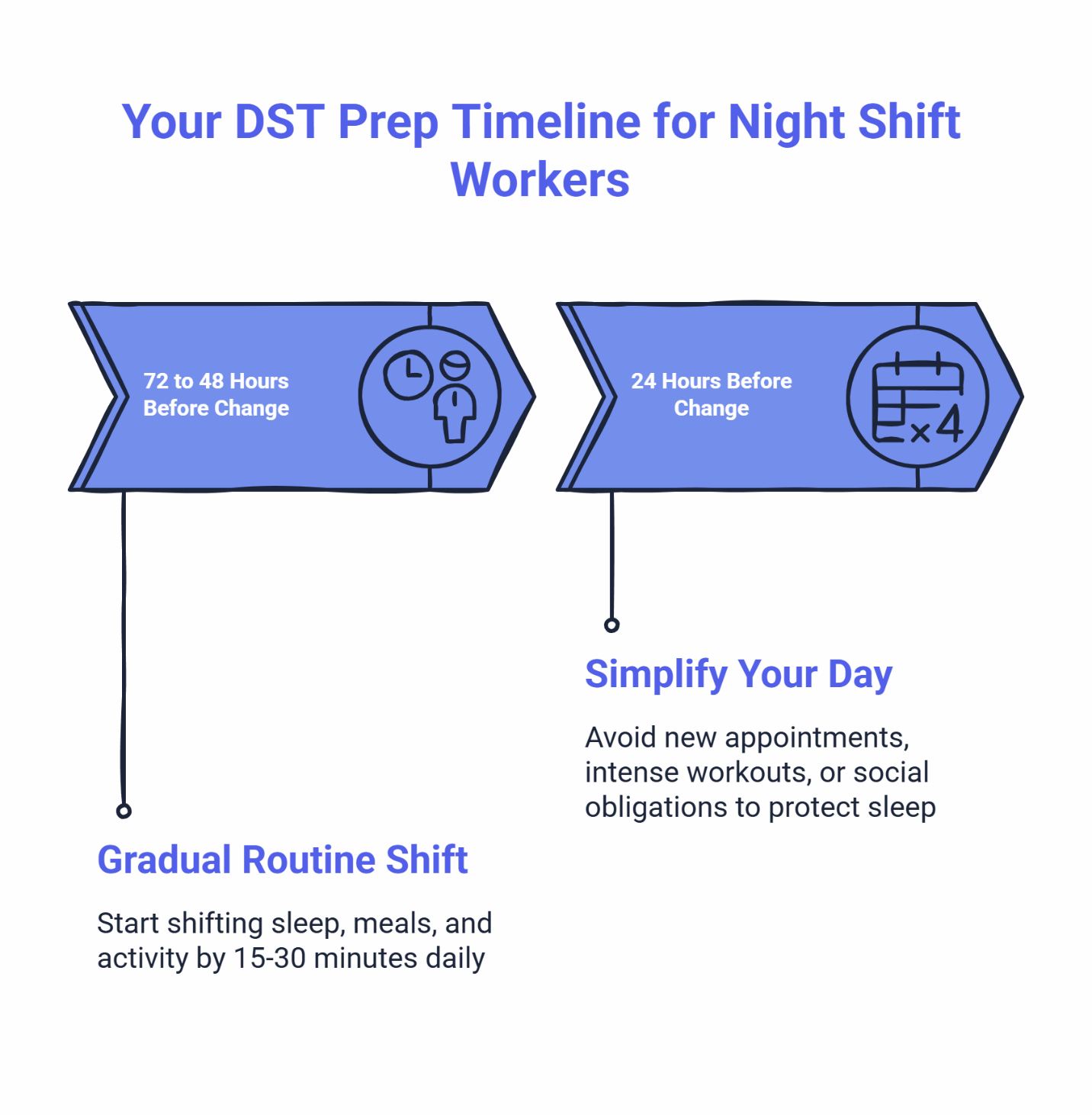
72 to 48 Hours Before the Change
Start shifting sleep-related routines by 15 to 30 minutes in the direction of the upcoming change.
This includes more than just when you lie down. Your body notices meal timing, activity timing, and light timing. DST adjustment works better when those cues point in the same direction.
For the spring change, move your sleep window, wake time, wind-down routine, first meal after waking, and caffeine cutoff a little earlier each day. For the fall change, move those same anchors 15 to 30 minutes later each day.
A simple way to think about it:
- Wake time: Move it slightly earlier or later depending on whether clocks spring forward or fall back.
- Meals: Shift your main meals by the same increment. Eating cues help anchor your internal clock.
- Caffeine cutoff: If you normally stop caffeine six hours before sleep, keep that buffer but move the cutoff time with your adjusted schedule.
- Wind-down routine: Start dimming lights and reducing stimulation a little earlier or later than usual.
- Blackout setup: Make sure your sleep environment is ready. Check that curtains block light fully and that your room will stay dark during your adjusted sleep window.
The goal is to give your body a head start so the clock change doesn’t land all at once.
24 Hours Before the Change
Simplify your day. Get boring on purpose. Don’t stack new variables on top of the time change.
If you can avoid scheduling appointments, intense workouts, or social obligations that cut into your pre-sleep wind-down, do it. This isn’t about being rigid. It’s about protecting the one recovery sleep block that matters most.
If you’re working the night that crosses the DST transition, use this day to set yourself up:
- Confirm your blackout curtains are working.
- Prep meals so you’re not making food decisions while exhausted.
- Decide your caffeine cutoff in advance.
- Let anyone in your household know you need a protected sleep window after the shift.
The more decisions you remove, the easier it is to stay steady.
What to Do During the Shift That Crosses the Clock Change
NIOSH guidance on light exposure suggests using brighter light strategically during the first part of a night shift to support alertness. Later in the shift, reducing light exposure can make it easier to sleep afterward.
Practically, this means:
- If your workplace allows it, position yourself near brighter light sources earlier in the shift.
- In the final hours before you leave, reduce exposure to bright overhead lights where possible.
- Wear sunglasses on the drive home if the sun is up. This protects your wind-down by limiting bright-light cues that tell your body to wake up.
A note on driving: If you feel very sleepy heading home, don’t push through. A short nap in your car before driving, or a ride from someone else, is safer than forcing it. The CDC notes that DST transitions can increase drowsy-driving risk, and shift workers are already more vulnerable to fatigue-related incidents.
How to Handle the First Sleep Block After the Change
This sleep session matters more than the next few. Don’t try to “catch up” on everything at once. Don’t chase a perfect sleep score.
Night-shift workers often sleep less overall and get poorer-quality sleep than day workers. CDC/NIOSH guidance notes night workers usually get less sleep and must ruthlessly protect their scheduled sleep window to avoid chronic sleep loss.That makes protecting this first recovery block even more important.
Focus on three things: darkness, consistency, and enough time in bed.
When you get home:
- Keep lights dim.
- Avoid screens for at least 30 minutes before lying down.
- Eat lightly if you’re hungry, but don’t turn the hour after work into a full second day.
- Stick to the adjusted plan instead of improvising.
If you wake earlier than intended, don’t panic. Lie still in the dark for 15 to 20 minutes. If you can’t fall back asleep, get up quietly, avoid bright light, and try again later rather than tossing and turning.
How to Steady Your Rhythm Over the Next Two Days
The first two days after the change are about consistency, not perfection.
Track a few simple signs:
What to Notice | What It Tells You |
|---|---|
Ease of falling asleep | Is your body accepting the new timing? |
Wake-up clarity | Are you waking groggy or reasonably alert? |
“Stuck” feeling | Does your body still feel locked on the old schedule? |
Drive home or early-shift alertness | Are you dragging harder than usual? |
If things are improving, stay the course. If you’re still struggling after three or four days, that’s useful information. It may mean the issue is bigger than just the DST adjustment.
How Light, Darkness, and Routine Timing Can Make the Switch Easier
Your circadian system pays attention to cues. Light is one of the strongest. Random light exposure can make a rough week worse. Strategic light exposure can make it more manageable.
NIGMS notes that light at night, including light from devices, can confuse biological clocks. That’s why timing matters.
When to Use Bright Light
Bright light tells your body it’s time to be awake. For night-shift workers, this means using light strategically:
- Early in your shift: Brighter light supports alertness when you need it most.
- After waking from your main sleep: If you’re trying to shift your clock later, some bright-light exposure after waking can help.
You don’t need special equipment. Being near well-lit areas, or stepping outside briefly if it’s daylight, can work.
When to Protect Darkness
Darkness tells your body it’s time to wind down. Protect it:
- Before your sleep window: Dim household lights for at least 30 to 60 minutes before bed.
- During sleep: Blackout curtains or a quality sleep mask are essential. Any light leak can disrupt your rest.
- On the drive home: Sunglasses block the bright morning light that would otherwise signal “wake up.”
How Blackout, Caffeine Cutoff, Meals, and Screens Fit the Plan
Think of these as timing tools, not moral tests. They’re part of the same system:
- Blackout: Non-negotiable for daytime sleep. If your current setup lets light through, fix it before DST hits.
- Caffeine cutoff: Keep at least a six-hour buffer before your intended sleep time. When you shift your sleep window, shift the cutoff too.
- Meals: Eating at consistent times helps anchor your internal clock. Don’t skip meals, but avoid heavy eating close to sleep.
- Screens: The blue light from phones and tablets can delay sleep onset. Put them away 30 minutes before bed, or use a red-light filter if you must check something.
Where Medication-Supported Sleep Fits In
For some shift workers, non-controlled sleep medications provide a reliable anchor during abrupt schedule changes like DST. Options like trazodone, hydroxyzine, and clonidine work differently than benzodiazepines or Z-drugs. Because they are non-controlled substances, they generally avoid the specific addiction and abuse risks associated with Schedule IV controlled medications, though patients must still be monitored—abrupt discontinuation of medications like clonidine, for example, can cause adverse rebound effects. Many shift workers find them helpful for stabilizing rest when schedules get unpredictable.
SleepScriptMD offers these non-controlled options as first-line tools for eligible patients. The goal isn’t to replace good sleep habits. It’s to provide reliable support when your schedule makes consistent rest genuinely difficult.
If you’re already using a medication like this as part of a care plan, the DST transition is a reasonable time to think about timing. When you take the medication relative to your adjusted sleep window matters. Small shifts in timing, aligned with your prep plan, can help the medication support your transition rather than working against it.
Questions like “Should I take my medication 15 minutes earlier during DST?” or “What if I’m rotating to a different shift pattern next week?” are best handled by a provider who knows your specific situation. SleepScriptMD offers physician-led care, and many patients can complete the process online in most states.
For more on timing principles, see Non-Controlled Sleep Medications Timing Windows.
When This Is Not Just a DST Problem
DST makes existing sleep problems worse. But sometimes what looks like a DST adjustment issue is actually a sign of something that needs different care.
Snoring, Gasping, or Breathing Pauses
If you or a partner have noticed snoring, gasping, or pauses in breathing during sleep, that’s a red flag for possible sleep apnea. This condition requires testing before medication decisions are made.
At SleepScriptMD, readers who report these symptoms can still begin the intake process, but an at-home sleep test is required before any medications are prescribed. Results need to be reviewed first.
Possible Narcolepsy
Falling asleep unexpectedly during the day—especially during activities like talking or driving—is different from normal shift-work fatigue. So is sudden muscle weakness during strong emotions, or feeling paralyzed when falling asleep or waking up.
These symptoms point to possible narcolepsy, which requires in-person evaluation with a sleep specialist. Online treatment isn’t appropriate for this.
Possible REM Sleep Behavior Disorder
If you physically act out dreams—yelling, kicking, or punching during sleep—that’s a sign of REM sleep behavior disorder. This condition is important to identify because some common sleep medications can worsen or unmask symptoms.
RBD requires a video sleep study for diagnosis and is outside the scope of online insomnia treatment.
Possible Restless Legs Syndrome
An uncomfortable urge to move your legs at night, especially when resting, can signal restless legs syndrome. This condition often has underlying causes like iron deficiency, kidney issues, or nerve damage that need to be ruled out before treatment.
RLS requires in-person evaluation and lab work before it can be safely treated.
If any of those sound familiar, the next step is proper evaluation, not pushing harder.
If DST Keeps Disrupting Your Sleep
If you’ve tried the prep timeline and your sleep still isn’t recovering after a few days, it might be worth a closer look.
Take a Quick Sleep Quiz
The Sleep Clarity Quiz takes about two minutes and helps identify what’s actually affecting your rest. It’s based on clinical sleep tools, and you’ll get a printable PDF with clear next steps. It’s not a diagnosis, but it can help you understand whether your situation is straightforward schedule disruption or something that needs more attention.
If you want something even faster, the 6-Second Sleep Check is a quick gut check on whether your sleep needs support. Five questions, immediate feedback.
Ready to Start Treatment?
If you’re an adult between 18 and 65 without major medical complications, you may be a good fit for SleepScriptMD’s physician-led care. The process is straightforward: complete a brief intake, get reviewed by a board-certified physician, and if eligible, receive a prescription sent to your pharmacy—often the same day in most states.
Start your sleep treatment here, or view pricing and plan options to see what works for you.
Disclaimer: This article provides general information about Daylight Saving Time disruption for night-shift sleep schedules for educational purposes. Individual circumstances vary significantly based on factors like your shift pattern, your sleep timing, light exposure, medication timing, and any underlying sleep or medical conditions. For personalized guidance tailored to your night-shift sleep needs, consult with a qualified professional.
Our Editorial Process:
Our expert team uses AI tools to help organize and structure our initial drafts. Every piece is then extensively rewritten, fact-checked, and enriched with first-hand insights and experiences by expert humans on our Insights Team to ensure accuracy and clarity.
By: The SleepScriptMD Insights Team
