📌 Key Takeaways
Non-controlled sleep medications like Trazodone, Hydroxyzine, and Clonidine work effectively when you protect them with consistent timing and avoid stacking sedating substances.
- Timing Consistency Prevents Grogginess: Taking medication in the same 30-minute window nightly and allowing 7-8 hours before waking minimizes next-day sedation.
- Avoid Sedative Stacking: Combining your prescription with alcohol, OTC sleep aids, or sedating supplements creates prolonged morning fog.
- Three Non-Addictive Options: Trazodone maintains sleep through the night, Hydroxyzine calms anxious racing thoughts, and Clonidine addresses sympathetic overactivity.
- Track Your Morning Clarity: Rating how you feel (1-10 scale) each morning for the first week gives clinicians data to fine-tune your plan quickly.
- State Regulations Vary: Many states allow asynchronous care through intake form review, while others require brief video or audio visits before prescribing.
Simple habits protect medication effectiveness better than perfection.
Adults with persistent insomnia seeking physician-supervised, non-controlled prescription options will find practical safety guidelines here, preparing them for the detailed medication information and treatment process that follows.
It’s 11:47 PM. You have a presentation at 9 AM. The melatonin didn’t work. The breathing exercises didn’t work. You’re scrolling through search results, hoping this time will be different.
If you’re using a prescription sleep aid under clinician guidance, the goal isn’t to feel “knocked out”—it’s to get predictable sleep and wake up clear. Think of prescription sleep aids as installing a reliable sleep auto-pilot. When the system works, you follow your pre-bed routine, take your medication at a consistent time, and wake up ready for the day. But the auto-pilot only works if you protect it—skip the alcohol, avoid late caffeine, and don’t experiment with your timing window on a whim.
Why These Medications Work Well
Non-controlled sleep medications like Trazodone, Hydroxyzine, and Clonidine are prescribed routinely by sleep specialists because they’re effective, non-addictive, and well-tolerated by most patients. When you follow straightforward timing and safety guidelines, these medications help you fall asleep faster, stay asleep longer, and wake up functional. The biggest mistakes are usually timing and stacking sedating substances (like alcohol or other drowsy meds)—not the medications themselves. The rules below keep your morning clarity intact and help you message your clinician when something feels off.
The Short Version: Your Avoid List to Protect Tomorrow Morning
While these medications are designed to clear your system by morning, next-day grogginess can often be managed by refining your timing or checking for interactions. Consistency helps your body adapt to the medication profile.
What to Avoid Tonight (So You Wake Up Clear)
Avoid | Why It Matters | Do This Instead | Ask Your Clinician When… |
|---|---|---|---|
Alcohol | Compounds sedation; disrupts sleep quality | Skip it on dosing nights | You’re tempted to drink or feel unusual effects |
Late caffeine (after 2 PM) | Blocks natural sleep signals for hours | Set a caffeine curfew | You’re still wired at bedtime despite timing |
Blue-light devices before bed | Stimulates alertness when you need calm | Use night mode or put devices away 30 min before | You can’t fall asleep even with medication |
Dosing at random times | Creates unpredictable wake times and grogginess | Pick a 30-minute window and stick to it | Your wake time varies by more than an hour daily |
Adding OTC sleep products | May cause additive sedation and side effects | Disclose all supplements/herbals to clinician first | You’re considering combining products |
Driving/machinery if groggy | May affect reaction time and functioning | Wait until you feel fully alert | You feel sedated the next morning |
Re-dosing in the night | May cause prolonged sedation and morning fog | Only if explicitly instructed by clinician | You wake up and can’t fall back asleep |
Sharing medications | Unsafe and illegal; meds are prescribed for you only | Keep in secure location | Someone asks to try your medication |
What “Interactions” Really Means (in Normal Language)
When your clinician talks about “interactions,” they’re describing three main situations that can make you feel foggy, dizzy, or off the next day.
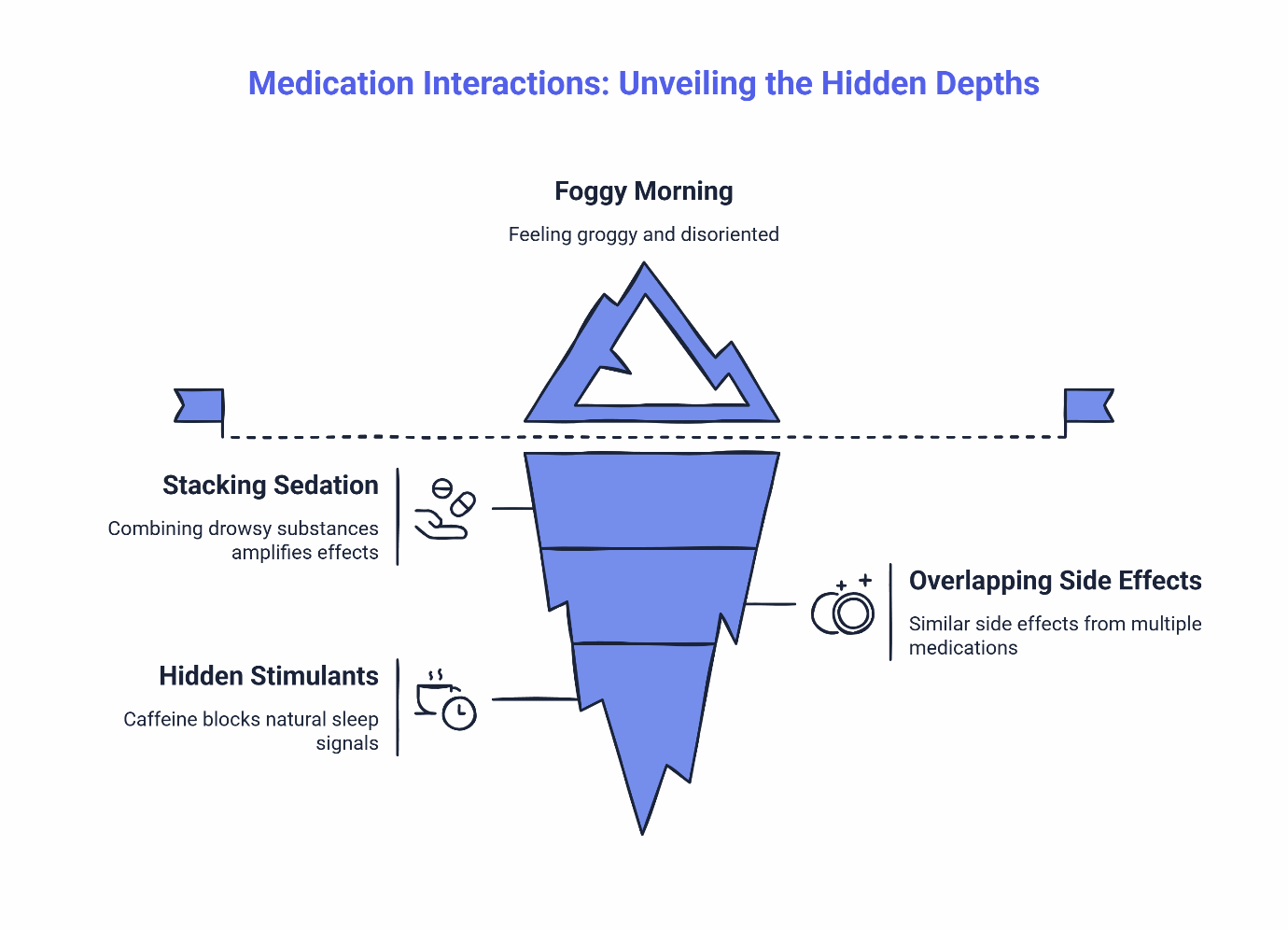
Stacking Sedation (Two Drowsy Things = One Foggy Morning)
This happens when you combine your prescription sleep aid with anything else that makes you drowsy—alcohol, antihistamines like Benadryl, certain herbal supplements like valerian root, or other prescription medications that list “drowsiness” as a side effect. Your body processes each sedating substance at its own pace. When you stack them, the combined effect can linger into your morning alarm, leaving you feeling like you’re moving through fog.
Overlapping Side Effects (Dizziness + Low Blood Pressure = Feeling Off)
Some medications can cause similar side effects—like dizziness, lightheadedness, or a drop in blood pressure. When you combine them, these effects can amplify. For example, if your sleep medication can lower blood pressure slightly and you’re also taking a blood pressure medication, standing up quickly in the morning might make you feel unsteady. This is why your clinician needs to know about every medication and supplement you take, even the over-the-counter ones you don’t think “count.”
“Hidden Stimulants” (Late Caffeine Blocking Your Sleep Signal)
Caffeine after 2 PM can still be in your system at bedtime, blocking the natural sleep signals your medication is trying to support. Even if you “feel fine” with afternoon coffee, the chemical is actively working against your treatment. Same goes for energy drinks, pre-workout supplements, and even some pain relievers that contain caffeine.
Interaction Quick Reference
Interaction Type | What It Feels Like | What to Do |
|---|---|---|
Sedative stacking | Extreme grogginess, confusion, memory gaps | Tell your clinician about all drowsy meds/supplements |
Overlapping side effects | Dizziness when standing, feeling “off” | Review your full med list with clinician |
Hidden stimulants | Can’t fall asleep despite medication | Cut caffeine after 2 PM |
Medication-Specific Watch-Outs (Examples)
SleepScriptMD focuses on non-controlled sleep medications like Trazodone, Hydroxyzine (Vistaril), and Clonidine. These medications work differently from controlled substances, but they still require the same careful timing and avoid-list hygiene.
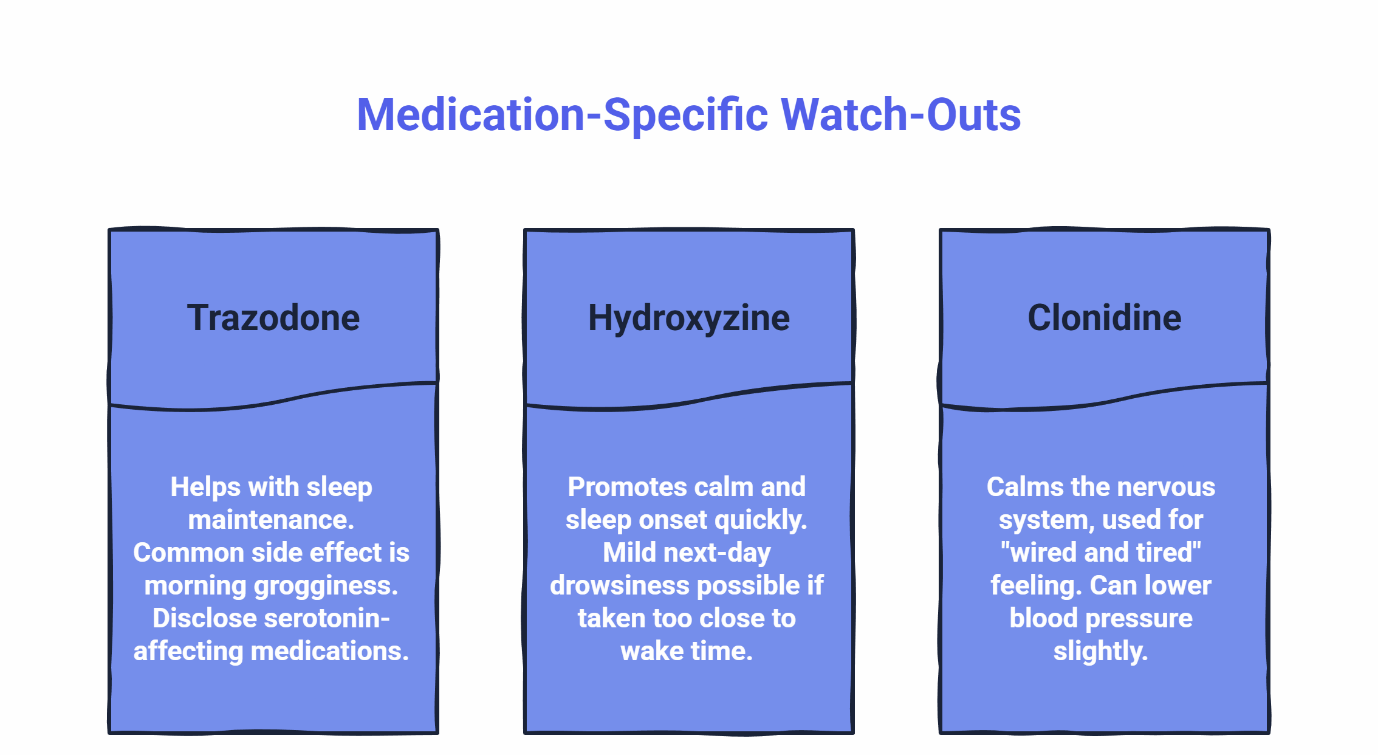
Trazodone
Trazodone helps with sleep maintenance—staying asleep through the night. Common side effects include morning grogginess or “hangover,” particularly during the first few days of treatment as your body adjusts. If you’re taking other medications that affect serotonin (like certain antidepressants), disclose this to your clinician, as combining them requires careful monitoring. Reviewing official medication guidance can help clarify side effects and cautions: MedlinePlus trazodone information.
Message your clinician if morning sedation persists across multiple days, or dizziness/lightheadedness shows up in a way that affects your daily activities.
Hydroxyzine
Hydroxyzine promotes calm and sleep onset, working quickly—usually within 15 to 30 minutes. Some people feel mild next-day drowsiness if they take it too close to their wake time (less than 7 hours before their alarm). Shifting your dose 15 to 30 minutes earlier often solves this. Official guidance is available at MedlinePlus hydroxyzine information.
Message your clinician if sedation feels excessive, or you notice confusion or impaired functioning the next day.
Clonidine
Clonidine calms the nervous system and is often used off-label for sleep disturbances associated with sympathetic overactivity (the “wired and tired” feeling). It can lower blood pressure slightly, so your clinician will check if you’re prone to dizziness or taking other blood pressure medications. Many patients report it causes less “heavy” morning brain fog compared to other sedatives, though some mild lethargy is possible as your body adjusts. Consistency in timing is key to minimizing this. Background pharmacology and cautions are summarized at NCBI Bookshelf clonidine overview.
Message your clinician if dizziness is persistent, you feel faint, or the plan affects normal daily functioning.
The pattern across all three: timing consistency and avoiding sedative stacking are what keep your mornings clear. When used correctly, these medications are effective tools for restoring healthy sleep patterns.
The First-Week Rule: Consistency Beats Experimentation
The first seven nights on a supervised sleep plan are about building predictability, not perfecting your sleep immediately. Your goal is to establish a baseline so your clinician can fine-tune the plan safely.
Change One Thing at a Time
If you adjust your dose timing, don’t also add a new supplement or change your caffeine routine that same night. When you change multiple variables at once, you won’t know which one caused the improvement—or the problem. This rule protects you from guessing games and keeps your clinician’s adjustments precise.
Track Your Morning Clarity Score (1–10)
Each morning, rate how you feel on a simple scale: 1 = couldn’t function, 10 = completely clear and energized. You’re not aiming for a perfect 10 every day. You’re looking for a pattern—most mornings should land around a 7 or 8 by the end of the first week. If you’re consistently below a 5, message your clinician. That’s useful data for adjusting your plan.
Pick a Timing Window and Lock It In
Choose a 30-minute window before your target bedtime (for example, between 10:00 and 10:30 PM) and take your medication at the same time every night. Don’t dose at 11:43 PM one night and 9:15 PM the next. Your body needs a repeatable cue to sync with the medication’s effects. Anchor your timing to a consistent pre-bed routine—like brushing your teeth or dimming the lights—so it becomes automatic.
For a structured self-check on your sleep pattern, take the 2 Minute Sleep Clarity Quiz.
When to Contact a Clinician (and When It’s Urgent)
Your clinician expects you to reach out if something feels off. That’s not “bothering” them—it’s using the system correctly.
Message Your Clinician If:
- You’re experiencing persistent next-day sedation that doesn’t improve after adjusting your timing
- You feel unusually dizzy or lightheaded, especially when standing
- You notice mood changes, confusion, or memory gaps
- Your sleep isn’t improving after the first week of consistent use
- You’re tempted to combine your prescription with other sedating products (OTC sleep aids, alcohol, or herbal supplements)
Seek Immediate Medical Care If:
You experience severe symptoms like difficulty breathing, chest pain, or signs of a severe allergic reaction.
The difference is straightforward: message your clinician for adjustments and concerns; seek immediate care for severe symptoms.
How SleepScriptMD Keeps This Safety-First
This isn’t a “skip the doctor” shortcut. Every prescription goes through a safety screen and clinician review to make sure supervised sleep medication is appropriate for you.
Eligibility Screening
You’ll complete a secure online intake that asks about your medical history, current medications, and sleep patterns. SleepScriptMD can only treat patients at low risk of side effects or complications—adults ages 18 to 65 with no major medical, mental health, or substance use conditions that could make sleep medications unsafe.
Sleep Testing When Needed
If you’ve been told you snore, gasp, or stop breathing during sleep, you’ll need to complete an at-home sleep test before any treatment can begin. Medications are not prescribed until your test results are reviewed. Most patients begin testing within just a few days.
Clinician Review and State Variation
A licensed physician or nurse practitioner reviews your intake. In many states where regulations allow, this happens through secure, asynchronous care (a thorough intake form review). In states requiring synchronous care, a brief video or audio visit will be seamlessly scheduled. Either way, a real clinician makes the final call on whether a prescription is appropriate, and no prescriptions are auto-generated.
Your prescription is sent electronically to your pharmacy of choice, and you’ll receive guidance on timing, what to avoid, and when to check in. Refills are simple—most patients continue with monthly or quarterly plans and can adjust or cancel anytime.
Want to see how the process works? Compare AI-assisted vs virtual appointments or check current pricing options.
Ready to get matched with the right medication? Start your sleep treatment and complete your secure assessment in under 10 minutes.
FAQs
What if I took my medication too late?
If you realize you dosed later than your usual window and you have an early morning commitment, don’t panic. Set an extra alarm, allow yourself more time to wake up fully, and avoid driving or operating machinery until you feel completely alert. Message your clinician about the timing issue so they can help you adjust your routine going forward.
Can I take OTC sleep products along with my prescription?
Not unless your clinician explicitly approves it. Combining your prescription with over-the-counter sleep aids like diphenhydramine (Benadryl), doxylamine (Unisom), or herbal supplements like valerian root creates a sedative-stacking situation. Always disclose what you’re taking—even “natural” products—so your clinician can assess safety.
Why do I feel groggy the next day?
The most common causes are timing (dosing too late or too close to your wake time) and interactions (stacking sedating substances). Less commonly, the dose itself may need adjustment. Track your morning clarity score for three to five days, note your exact dosing time, and share this pattern with your clinician. They can usually solve it with a simple tweak.
How long should I wait before driving in the morning?
Wait until you feel fully alert and clear-headed. If you’re experiencing any grogginess, dizziness, or “foggy” feeling, do not drive. For most people using medications like Trazodone or Hydroxyzine, this means waiting at least 7 to 8 hours after dosing. If you consistently feel impaired in the morning, your timing or dose likely needs adjustment.
What if I have to wake up early tomorrow?
Don’t take your medication. If you know your sleep window will be shorter than 7 hours, skip that night’s dose. Taking your medication and then waking up after only 5 hours will leave you feeling sedated and less functional. Consistency matters, but protecting your morning matters more.
How do I know if this treatment is unsafe for me?
The screening protocol flags conditions that typically require in-person evaluation—such as symptoms of narcolepsy, REM sleep behavior disorder, or restless legs syndrome—as well as other contraindications that need specialized care. These conditions require specialized evaluation and testing that can’t happen online.
What should I track during the first week?
Track three things: your exact dosing time each night, your morning clarity score (1–10), and any side effects or unusual symptoms. This simple log gives your clinician the data they need to fine-tune your plan quickly and safely.
Ready to Start Sleeping Better?
Non-controlled sleep medications like Trazodone, Hydroxyzine, and Clonidine help thousands of patients sleep better every night—without the addiction risks of controlled substances. When you follow simple timing and safety guidelines, these medications work effectively to restore healthy sleep.
Start your sleep treatment • Take the 6 Second Sleep Check • Explore treatment options
Disclaimer: This article is educational and not a substitute for medical advice. Prescription sleep medications should only be used under the guidance of a licensed clinician. If you think you may be experiencing a medical emergency, call 911 or seek emergency care.
Our Editorial Process
Our expert team uses AI tools to help organize and structure our initial drafts. Every piece is then extensively rewritten, fact-checked, and enriched with first-hand insights and experiences by expert humans on our Insights Team to ensure accuracy and clarity.
About the SleepScriptMD Insights Team
The SleepScriptMD Insights Team synthesizes complex sleep medicine topics into clear, helpful guides. Content is educational and not a substitute for medical advice.